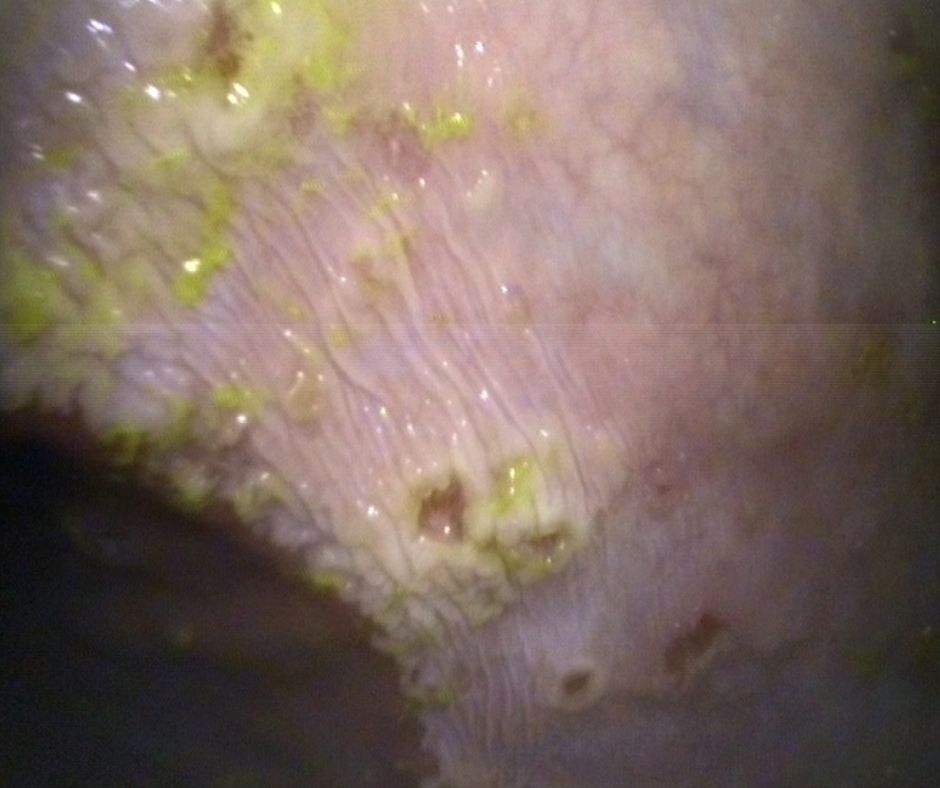
If your vet confirms your horse has ulcers by gastroscopy (scoping) he MUST be medically treated. Feeding a horse with ulcers needs careful consideration, however, as ulcers can be caused by many factors. One of the most important factors is nutrition and ongoing nutritional management. It’s vital to get this right if you want to avoid reoccurrence.
Feeding Ulcer Prone Horses – What are the different types?
Squamous type ulcers
Most commonly diagnosed in Thoroughbreds. They affect the top, white-coloured third of the stomach and reflect increased acid exposure of the tissue. These ulcers form quickly and are consistently associated with changes in appetite, slowed eating and poor performance. Inconsistent changes in behaviour and/or attitude can also occur.
Squamous ulcers can occur with daytime forage deprivation, lack of access to water, high-starch diets, pelleted feeds, straw feeding. Additionally, intense exercise, travel, a change in housing and lack of daily horse to horse contact can have an impact.
Treatment with an equine formulation of the acid suppressant drug Omeprazole is consistently very effective, with most lesions healing within 14-28 days.
Complete healing occurs in up to 80% of squamous cases. Gastroscopy should ideally be repeated, but if the horse has responded well then this can be skipped and the horse put onto maintenance treatment for two to three months. Simply stopping all treatment at this point is associated with a high ulcer recurrence rate (approximately 80% within 6 weeks).
Glandular ulcers
They affect the pink bottom two-thirds of the stomach, in particular the final part. They’re more commonly seen in Warmbloods. Ulcers here form slowly and reflect failure of the mucus coat that protects glandular tissue from acid. It’s likely that several different causes – physical, toxic, bacterial or physiological – contribute to this failure. The clinical signs are more variable and may or may not include appetite change and/or weight loss. Some horses may start to resent the girth being tightened but this isn’t specific.
Treatment with Omeprazole alone is much less effective than in cases of squamous disease (25% healed after 28-35 days). Instead, a combination of Omeprazole and the mucosal protectant Sucralfate is used leading to a 68% healing rate. It’s also important to reduce the horse’s exposure to stress. Recent research has even shown that giving two days off work a week can be really helpful in reducing risk.
Hindgut Ulcers
There’s a lot of debate as to what ‘hindgut ulcers’ actually are. The study originally performed to identify hindgut ulcers used horses from abattoirs without any clinical history. This meant the relevance of the lesions detected was unclear.
A hindgut disease more commonly understood is inflammatory bowel disease (IBD). In this condition large portions of the hindgut become inflamed and thickened, even shedding part of their surface layers. This causes weight loss, intermittent diarrhoea and/or recurrent colic. It rarely affects behaviour or performance.
Diagnosis of IBD is made by a combination of abdominal ultrasound and blood tests. The blood tests will identify low protein levels, absorption studies and intestinal biopsy. Treatment involves 3 months of the anti-inflammatory corticosteroid prednisolone, and is successful in 70% of cases.
Are all Horses at Risk?
Racehorses are clearly at greatest risk because they work at greater speeds and are typically fed very little fibre. The link between exercise and ulcers, however, suggests that all horses that are worked regularly could be at risk so this would include dressage and event horses, as well as showjumpers.
Summary
Whatever treatment path you go down, keep it up for at least 2-3 months. Get your horse re-scoped to check the healing progress. It may hurt the pocket, but it’ll hurt even more if you aren’t consistent and the ulcers never clear up!
Feeding a horse with ulcers will mean that feeding practices will have to change. Your horse should be kept away from grain/cereal hard feeds. Other sweet feeds which can be too acidic may irritate ulcers further. However, this change needn’t be the end of the world if your horse is in hard work.
Tips for feeding ulcer prone horses to help manage and reduce reoccurrence:
- Feed as much fibre/forage as possible at a minimum of 1.5% of body weight (dry matter) per day.
- Don’t leave your horse for prolonged periods without forage.
- Avoid stalky forage being the sole or predominant forage source.
- If extra energy is needed look for feeds that have restricted starch and sugar levels and added oil rather than cereals.
- Aim to feed < 1g/kg bodyweight of non-structural carbohydrate (NSC: starch plus water-soluble carbohydrate) per meal. Preferably try to spread meals across the day – multiple small meals are better than one or two large ones.
- Add chopped fibre to every meal. Lucerne is particularly useful as it’s been shown to help buffer gastric acid.
- Avoid very stalky, sharp chopped fibre which can increase the risk of damage to the stomach wall.
- Provide a small chopped, fibre-based meal or access to forage before exercise. This helps to reduce gastric acid splashing up onto the sensitive stomach wall.
- Turn out to pasture as much as possible.
- Provide access to water at all times.
- Avoid using electrolyte pastes.
- Provide some form of forage while travelling.
A Fibregenix balancer plus non-cereal calorie sources, eg lucerne, and/or oil will also provide a low starch option. This can play a valuable part in feeding hard-working ulcer prone horses. One major benefit is it will enable you to limit the need for large amounts of hard feed by boosting essential nutrient intake and maximizing fibre digestion. Speedibeet or Fibrebeet is also a good choice. There is evidence that the pectin content of sugar beet can have an action similar to mucous. This will help line the stomach and protect it against acid attack.
A high omega 3 anti-inflammatory essential fatty acid oil such as cold-pressed linseed is also useful.
Never underestimate the amount of work that a horse can do on a high fibre diet. Once ulcers are cleared, with ongoing preventative management it may be possible to reintroduce small quantities of grain feed supplemented alongside the Fibregenix balancer.
Sound familiar?
“My dressage horse isn’t his usual self. He’s been girthy, hates having his rugs on, fidgets when I tack him up, is fussy about having his feet picked out with his saddle on He’s started moving away when I try to get on and is reluctant to go off my leg as much as he was. All of these signs make me think he might have gastric ulcers so the vet is coming out to check him over and confirm if this is the case…”
It’s one of the most common questions we are often asked. How should I feed my hard-working competition horse if he’s been diagnosed with gastric ulcers?
Speak to/email our equine Nutrition consultant Anita for a friendly chat about an ulcer prevention strategy and a diet audit, We are here to help you: 0408920707 or anita@fibregenix.com.au
Reviewed and amended April 2021